Can Natural Remedies Succeed in health and wellness Where Modern Medicine Fails?
Naturopathic medicine is an eclectic approach to health that incorporates traditional diagnostic techniques with natural therapeutic modalities. Emerging in the early 1900’s as a unique medical discipline, naturopathic medicine is presently experiencing unparalleled interest as a complete approach to optimal health.
NEW AT LOTUSRAIN – PLAQUEX IV
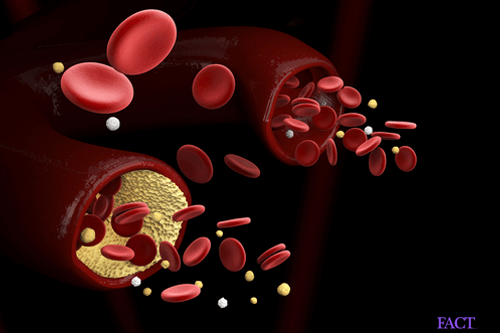
We are excited to announce our latest addition to our widely-varied IV infusion menu. Have you been diagnosed with a high Calcium Score? Are you concerned about plaque buildup in the arteries?
These can be addressed with the Plaquex Infusion. Contact the office for further details.
OUR SERVICES
Primary Care
IV Therapy & Nutrition
Integrative Oncology & Cancer Care
Prevention & Optimal Health
LotusRain Naturopathic Medicine and IV Clinic
LotusRain Naturopathic Medicine and IV Clinic
Our goal in utilizing Naturopathic Medicine is to explore the full scope of physical, emotional, environmental, mental, social, and spiritual influences that affect each person individually. We use conventional and specialized functional testing to help diagnose, but utilize natural modalities to treat. Our principles are always to seek the underlying cause and treat the whole person.
Our dedicated team of licensed naturopathic doctors invites you to a positive, light-filled space where we help you optimize your health.
Book a Free
20-min Consultation
Do you have any questions?
If you’re a first time patient, we offer a FREE 20 minute consultation! Click below to schedule an in office or phone consultation.
MEET THE PROVIDERS OF LOTUSRAIN

Circumstances led Dr. Hilewitz to pursue a degree in Acupuncture, graduating 25 years ago, which she taught and practiced intensively for 10 years. Through learning and integrating the Chinese medicine philosophy, Dr. Hilewitz came to understand healing and the human experience differently, with a deep recognition that we live on all 4 planes of existence – physical, mental, emotional and spiritual and cannot separate the physical from the mind and the body, leading to interconnectedness.

Chinese Medicine is a deeply healing and relaxing treatment modality, that heals the root of a problem, not just the symptoms. Chinese Medicine can help many conditions, including, but not limited to: stress, anxiety, insomnia, digestive issues, female reproduction issues, adjunctive therapy to chemotherapy or radiation, common cold, allergies, and even immunity boosting.

Dr. Dubroff utilizes a broad range of therapies to assist nature in healing what imbalances us. Some of these therapies he uses are clinical nutrition, IV therapy, botanical medicine, classical homeopathy, bio-identical hormones, counseling, hydrotherapy, peptide therapies and prolotherapy and other pain curative procedures.
“I feel blessed to have had the opportunity to study naturopathic medicine and likewise continue to broaden my knowledge of the art and science of medicine every day! Even more so to be honored by a place in people’s lives to assist them in health, healing and discovery. To me there is no place equal on this planet as to know you have helped someone!”


His first seven years of practice included studying the energy healing of the Kahuna with the High Priestess of the Hawaiian Island. In 1994, at an unprecedented event in an ancient temple ceremony at Pu’uhonua, Hawaii, Steve was taken into his Kahuna’s lineage and given the name ‘Kalamakua’ meaning Ancient Wisdom. Steve received his Advanced Rolfing Certification in 1995 in Sao Paulo, Brazil and is currently practicing in both Phoenix and San Diego, dedicated to the healing of the planet.